HpVac-R13 is the derived from a natural immunomodulatory protein with strong epidemiological evidence of protecting humans against asthma and other allergic diseases.
In 2015, HpVac was selected as one of 6 most interesting candidates out of a pool of over 200 development projects.
HpVac-R13 is the optimized, recombinant version of a protein secreted by Helicobacter pylori, a constituent of the gastric microbiota, that protects itself against elimination by modulating the human host’s immune system. H. pylori unexpectedly provides protection against a number of human allergic and inflammatory diseases, including asthma, atopic dermatitis and hay fever.
Multiple in vitro and in vivo studies have confirmed the molecule's therapeutic potential.
HpVac-R13 has been administered orally, intraperitoneally and intranasally to mice with no unexpected side effects. Chronic exposure to HpVac-R13 and/or its variants has demonstrated its excellent tolerability and lack of toxicity in humans.
The lead optimization phase of the development program has been completed, and HpVac is currently initiating the IND-enabling activities of the program.
Improved hygiene standards in developed and developing countries, while reducing the incidence of infectious diseases, also contribute to an increase of the incidence of allergic and autoimmune diseases (the "hygiene hypothesis")1). Lack of exposure to allergens in early childhood is thought to sway the immune system towards allergy-promoting responses, partly because an excessively sanitized environment modifies the composition of the individual microbiota.
1) Okada et al, 2010, The ‘hygiene hypothesis’ for autoimmune and allergic diseases: an update Clin Exp Immunol. 2010 Apr; 160(1): 1–9, Abstract
Lambrecht, B.N. and H. Hammad, The immunology of the allergy epidemic and the hygiene hypothesis. Nat Immunol, 2017. 18(10): p. 1076-1083.
Ege, M.J., The Hygiene Hypothesis in the Age of the Microbiome. Ann Am Thorac Soc, 2017. 14(Supplement_5): p. S348-S353.
Asthma is a chronic condition characterized by the narrowing and inflammation of the airways, resulting in breathing difficulties. It is considered the most common chronic and frequent non-communicable disease among children1) and affects 5% of the overall population. During an asthmatic attack, patients experience breathlessness as in- and outflow of air decreases. Undergoing an asthma attack is a debilitating experience, and asthma sufferers must often undergo significant lifestyle changes, including limiting their activities, to keep the disease under control and avoid attacks. The disease is particularly distressing for small children and their parents. Asthma kills about 1000 persons a day and is a global NCD priority2).
There is currently no known cure for asthma. Current treatments for severe asthma include anti-IgE, anti-IL13 and anti-IL4 therapies. Long-term symptomatic treatments include the use of long-acting beta2 agonists (LABA) and inhaled corticosteroids. Immunotherapy with anti-leukotrienes, anti-IgE and anti-IL5 is indicated for patients not responding to the above treatments, but side effects may be severe.
1) Van den Akker-van Marle ME. et al. Evaluation of cost of disease: assessing the burden to society of asthma in children in the European Union. Allergy 2005; 60: 140–149.
2) Global Asthma Report 2018
3) Global Strategy for Asthma and Prevention- (GINA)- update 2021
Atopic dermatitis is a chronic, pruritic, inflammatory skin disease which occurs most often in early infancy. Approximately 50% of cases persist in adulthood. AD often precedes asthma or hay fever in the affected individual. Its overall prevalence is 2.2% worldwide. It is characterized by intense itching in sudden flares and recurrent eczematous lesions as a consequence of excessive scratching with a risk of superimposed infections. External triggers such as exposure to dry air, sweating, stress, but also some foods may worsen the state of the patient. AD strongly impacts the quality of life and the psycho-social wellbeing of patients.

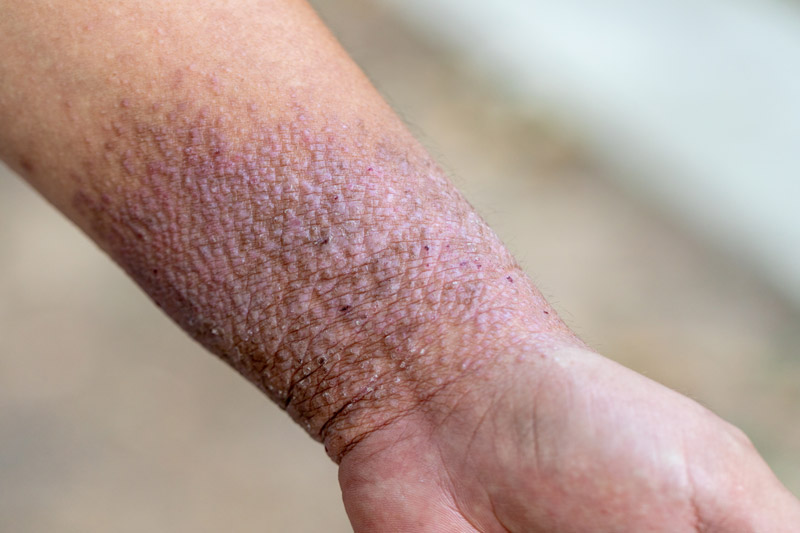
Currently, there is no cure for atopic dermatitis. Treatments with topical corticoids and, sometimes, antihistamines aim primarily at reducing discomfort and flares and preventing thickening of the skin. Individualized skin care programs and lifestyle changes to avoid trigger factors support medical treatments. Topical calcineurin inhibitors (non-steroidal anti-inflammatory agents) may be used as second-line therapy. Some cases react well to phototherapy, a treatment involving several visits per week at a specialized treatment center. Severe cases may be treated with immunosuppressants (e.g. cyclosporin or dupilumab), which typically cause significant side effects. There is an immediate, strong need to identify alternative cures and opportunities for disease prevention1).
1) Nutten S. Atopic dermatitis: global epidemiology and risk factors. Ann Nutr Metab. 2015;66 Suppl 1:8-16.
2) Kader, H.A., et al., Current Insights into Immunology and Novel Therapeutics of Atopic Dermatitis. Cells, 2021. 10(6).
Allergic rhinitis occurs when substances such as pollens, dust mites, pet dander and molds are inhaled through the nose, ingested, or come in contact with the eyes. The immune system mistakenly reacts to such substances as though they were intruders. Rhinitis may also be caused by irritants such as smoke or pollution. Hay fever affects 12-14% of the population of Europe and USA1)2). Allergic rhinitis symptoms include runny nose, watery eyes, coughing and itching of the nose and throat mucosa; it also generally causes headaches and fatigue due to sleeping difficulties. Individuals suffering from hay fever are more prone to allergic conjunctivitis and have a higher probability to develop asthma.

If the allergens are clearly identified, desensitization may bring long-term relief. Otherwise, corticosteroids, antihistamines, and decongestants, both as sprays or tablets, are generally used. All have side effects and are not indicated for use in neonatal and young pediatric patients. A further possibility is leukotriene receptor antagonists (LTRAs), which may increase the risk of infection.
1) V. Bauchau, S.R. Durham. Prevalence and rate of diagnosis of allergic rhinitis in Europe. European Respiratory Journal 2004 24: 758-764
2) Nathan R.A. et al. Prevalence of allergic rhinitis in the United States. JACI June 1997 Vol 99, Issue 6, Part 2, Pages S808–S814
IBD comprises two chronic inflammatory conditions. Crohn’s disease can affect any part of the intestinal track, whereas ulcerative colitis (UC) is the result of an abnormal reaction of the body’s immune system and affects mainly the colon and the rectum. The exact causes of the diseases are as yet undiscovered.
Patients suffering from IBD experience diarrhea, fever, fatigue, abdominal pain, blood in stools and weight loss. Both conditions impose significant lifestyle changes on patients, in an attempt to reduce the impact of the symptoms.
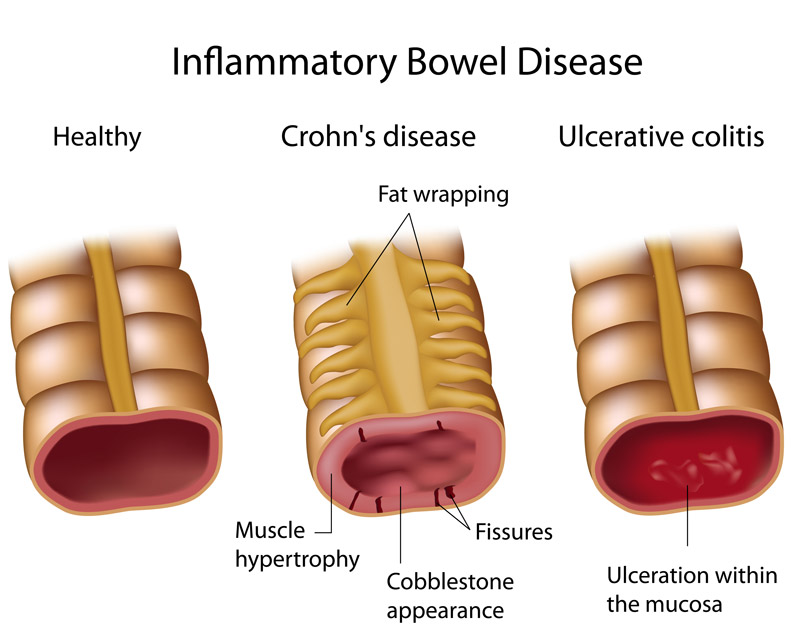
Current treatments for IBD include aminosalicylates, corticosteroids, and immunosuppressants (e.g. azathioprine or tacrolimus). Further possible treatments are biologic therapies such as anti-TNFs and anti-α4α7. Side effects can be serious. Treatments tend to be cost-intensive and may have to be prolonged indefinitely. In many cases, intestinal surgery is required to limit the damages caused by the disease.
Food allergies are defined as an immune response to food proteins and are the leading cause of fatal or recurring anaphylaxis in children and teenagers in Western countries. It is estimated that food allergies affect an average of 4% to 8% of children and 5% of adults and their prevalence appears to be rising like all allergic diseases. The most frequent food allergens are milk, eggs, peanuts, tree nuts, seafood, shellfish, soya, wheat and other foods. The symptoms include rashes, itching, swelling, diarrhea, or vomiting.

There are no approved treatments for food allergies, other than allergen avoidance and emergency treatment in cases of accidental ingestion. Oral immunotherapy (desensitization) strategies are also currently being developed as an option for food allergies. The patient’s quality of life is affected because of the fear of unintentional ingestion. Consequently, the need for new therapeutic approaches is mandatory.